2.1
Mechanism of Action
The
precise mechanism of action of emergency contraception in an individual
case cannot be certain as it depends on the time in the menstrual
cycle when the intercourse has occurred and when EC is taken.
The various postulated mechanisms depending
on the phase of cycle are:
- inhibition or delay of ovulation when
used prior to ovulation
- thickening of cervical mucus resulting
in trapping of sperms.
- direct inhibition of fertilization
- histological and biochemical alterations
in the endometrium leading to impaired inhibition or delay of
ovulation when used prior to ovulation endometrial receptivity
to implantation of a fertilized egg.
- alteration in the transport of egg, sperm,
or embryo.
- interference with corpus luteum function
and luteolysis
In summary, emergency contraception can
interfere with ovulation, fertilization or implantation depending
on the phase of menstrual cycle. EC is not effective once the
process of implantation of a fertilized ovum has begun and this
is the basis for the window-period of effective time frame.
2.2
Overview of methods
+
High dose estrogen
This was the first scientific method introduced
in the 1960s. The method consisted of diethylstilbestrol (DES) being
given in a dose of 50 mg per day for 5 days. Subsequently, the dose
was reduced to 10 mg per day. Association of DES with potential
effects on female offspring resulted in the discontinuation of use
of DES. Other estrogens like conjugated equine estrogen; ethinyl
estradiol and depot estrogens were also used. Though found effective
in preventing pregnancy, high-dose estrogen use is associated with
a high incidence of side-effects, especially nausea and vomiting.
Thus, women sometimes fail to complete the prescribed course of
treatment. Besides, menstrual pattern is disrupted following estrogen
use and the next period can be earlier with heavier flow. After
treatment failure, 10% of pregnancies are likely to be ectopic pregnancies;
thus estrogens alone are no longer used as Emergency Contraception.
+ Estrogen-Progestin
combination
In 1972
Yuzpe and his colleagues evaluated a combined ethinyl estradiol
and norgestrel pill each containing 50µg ethinyl estradiol
and 0.5 mg of norgestrel, 2 tablets being given twice, 12 hours
apart, within 72 hours of unprotected intercourse. This is commonly
known as Yuzpe Method. This has fewer side-effects compared to high
dose estrogen but still about 50% have nausea and 10- 25% vomit.
This is an easily available method. Regular dose oral contraceptive
pill can be used as post-coital pill in prescribed dose. A 4 pill
dedicated pack of combined ECP has been withdrawn from market in
certain countries following reports of higher efficacy and fewer
side effects with levonorgestrel.
+ Progestogens
Norgestrel as well as quingestanol have been
tried and shown to be effective over a range of doses. The side-effects
of progestogen-only pills are less than combination pills. In low
doses, progestogen may change the menstrual pattern. Trials have
shown progestogen-only pill containing 0.75mg levonorgestrel (LNG)
given in 2 doses, 12 hours apart within 72 hours of unprotected
intercourse, to be more effective with fewer side-effects compared
to Yuzpe method 6 . LNG has also been tried as 2 doses of 0.75mg,
12 hours apart upto 120 hours after sexual exposure, as well as,
as a single dose of 1.5mg again within 120 hours11.
Single dose has been reported to be as effective as two
doses 12 hours apart without increasing the side effect
and is more convenient to use. Currently LNG is the most
accepted method for emergency contraception.
+ Antiprogestogens
These are anti-implantation agents when given
post-coitally, menses inducers when given in luteal phase and abortifacients
when given in early pregnancy. Several antiprogestogens have been
tried. RU486 (mifepristone) has been found effective in a single
dose of 600mg, 100mg and 10mg when used as emergency contraception.
Current accepted dose for emergency contraception is 10mg.
In a comparative trial of RU486 with Yuzpe regimen, side-effects
were less common with mifepristone but menstrual disturbances occurred
more often12.
+ Antiestrogens
Danazol
has a direct luteolytic effect. A 400mg dose repeated 12 hourly
for 2 or 3 doses has been used with lesser side effects compared
to Yuzpe regimen13.
+ Centchroman
This an
antiestrogen with no progestational, androgenic or antiandrogenic
effects. It has been used as two 50 mg tablets given 12 hours apart
within 72 hours. Main side-effect is ovarian enlargement and delay
in menstruation causing confusion and tension. Adequate trials of
Centchroman as an effective emergency contraceptive are yet to be
conducted.
+ Intra-uterine
Device (IUD)
Insertion
of copper-T and copper-7 within 7 days of unprotected intercourse
have been reported as a highly successful method for post-coital
contraception. Copper-T is effective following even multiple coital
exposures during a short interval especially when the delay is beyond
120 hours, but less than 1 week, making hormonal methods ineffective.
IUD is particularly suitable for women who would like to continue
using it as a regular contraceptive. Contraindications to emergency
IUD use are the same as regular use.
Table
2 Comparison of Methods of Emergency Contraception
| Method & Dose |
Time after
Intercourse |
Failure
rate (%) |
Comments |
| No
contraceptive method |
- |
4-40
(overall 8) |
risk based on cycle
day |
| Vaginal
douching |
immediately |
15-20 |
very low efficacy |
| High
dose estrogen
Diethyl stilbestrol 50mg or
Ethinyl Estradiol 5mg X 5 days |
< 72 hours |
0.3-1.6 |
severe nausea &
vomitting,
failure to complete regimen |
Yuzpe’s
Regime (E+P) - Ethinyl
Estradiol 100 µg +
Levonorgestrel 0.5 mg |
<72 hrs, repeat after 12 hrs. |
O.2-3.2
(75-80% effective) |
risk of estrogen
use
low efficacy |
Danazol
800mgm X 3 doses
1200mg X 2doses |
72 hrs |
0.8-1.7 |
androgenic effect on repeated use |
| IUD
(CuT) |
5 days |
<1 |
risk of PID, unsuitable for nullipara,
infrastucture & training required |
| Centchroman
50mg 2 tablets |
72-120 hrs repeat
after 12 hrs |
to be evaluated |
menstrual delay |
Levonorgestrel
- 0.75 mg X2
1.5 mg X 1 |
upto 120 hrs, 0.75mg
(two doses 12 hrs apart) or 1.5mg (single dose) |
1.1 |
safe & effective
cheap |
Anti-Progestin
RU 486
(Mifepristone) 10mg single dose |
120 hrs |
1.1-1.3 |
menstrual delay,
risk of ectopic pregenancy
|
|
2.3
Effectiveness and probability of
conception
Overall
emergency contraception methods are less effective than regular
contraceptive methods. As a woman is not capable of conceiving throughout
cycle, EC effectiveness is better expressed in terms of ‘prevented
fraction’ of pregnancies after calculating the probability
of conception rather than the percentage failure.
The probability of conception after single
act of intercourse is approximatly 8%. Conception rate has been
calculated to be about 33% per cycle if intercourse occurs on average
every other day;14 if it occurs only once a week, the risk of
pregnancy is about 15%. Most women who have unprotected intercourse
on a single occasion, therefore, will not conceive. But the number
of fertile days of a menstrual cycle is difficult to quantify. The
sperms remain alive in the female genital tract and are capable
of fertilization for up to 5 days after ejaculation; the egg appears
to be capable of being fertilized for only about 24 hours. In a
recent study of couples actively trying to conceive with hormone
measurements to determine the timing of ovulation, the fertile period
lasted about six days, ending on the day of
ovulation14
. Acknowledging the small sample size in their study, however, the
authors concluded that a probability of conception of up to 12%
was theoretically possible if intercourse occurred on the day after
ovulation.
A normal fertile sexually active couple
not using contraception has an average monthly chance of conception
of 20-25% (counting only pregnancies that result in live births).
After fertilization, 25% of zygotes do not implant and
those that implant, a proportion (17%) is lost before a pregnancy
becomes clinically recognizable. Thus, in 42% cases no clinically
recognizable pregnancy results. Eight per cent of pregnancies are
lost spontaneously even after clinical confirmation13.
Accordingly, prospect of EC within 120 hrs of intercourse, interrupting
the natural development of a fertilized ovum appears very low, and
more so after a single act of unprotected intercourse. Therefore,
in a vast
majority of cases, EC addresses a theoretical or statistical, rather
than an actual, chance of fertilization having occurred and relieves
the woman’s apprehension of unwanted pregnancy considerably.
Efficacy
For calculating the prevented fraction the
formula used is:
1 - Observed Pregnancies
----------------------------------
Expected Pregnancies
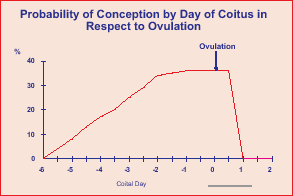
For calculating the expected pregnancies,
conception risk in menstrual cycle is calculated by probability
of conception on that day of cycle which has been calculated scientifically
(Fig 1). The day of ovulation is calculated by subtracting
14 days from the expected date of next period and depending on the
day of coitus in relation to this
day probability is estimated. Thus efficacy of EC in expressed in
2 ways
Overall pregnancy rate and
Prevented fraction of pregnancies
Table 3
The efficacy of different EC regimens
| |
Crude
pregnancy
rate (%) |
prevented
fraction (%) |
| Yuzpe Regimen6 |
3.2 |
75 |
| Levonorgestrel
tablet6 |
1.1 |
85
|
| Mifepristone
tablet12 (RU 486) |
0.9 |
85-90 |
| CuT IUD 6 |
0.1 |
99-100 |
|
2.4
Levonorgestrel (LNG) - the
dedicated method of choice
Levonorgestrel - two tablets of 0.75mg (single
pack) is specifically developed for emergency contraception. Though
a wide range of regular oral contraceptive pills can also be used,
it is believed that a dedicated product that is ‘a
product which is specifically packaged and labeled for use as emergency
contraception’ would ensure correct dosage, along
with trust of the client and service-providers towards emergency
contraception. Levonorgestrel is the preferred
method over Yuzpe regimen due to its higher efficacy and lesser
side effects6.
2.4.1 Dosage schedule and time frame
LNG ECP is available as a two pill pack each
tablet containing 0.75 mg of levonorgestrel. The pill can be prescribed
in two ways
single dose both tablets (total 1.5
mg LNG) to be taken together as a single dose within 120 hours of
sexual exposure
two dose regimen - one tablet to be taken
as soon as possible after intercourse but not later than 120 hours,
and second tablet 12 hours later.
2.5
Alternate methods for EC
2.5.1
Combined oral contraceptive pill
(Yuzpe Regimen)
Combined estrogen-progestin contraceptive
pills (COC) used in dosage so as to deliver 100 µg of ethinyl estradiol
plus 0.5 mg of levonorgestrel (or 1.0 mg norgestrel) as soon as
possible but optimally within 72 hours after unprotected intercourse,
twice at 12 hours interval.
As different COC formulations are available,
the number of tablets to be used can be decided according to Table
4.
Table 4
COC as EC
How many pills to be taken
| Brand Name |
Estrogen |
Progestrogen |
No. of tablets
to be used |
| Ovral |
Ethinyl
estradiol |
0.05
mg |
Levonorgestrel |
0.25 mg |
2+2 |
| Ovral
G |
Ethinyl estradiol |
0.05 mg |
Norgestrel |
0.5 mg |
2+2
|
| Ovral
L |
Ethinyl estradiol |
0.03 mg |
Levonorgestrel |
0.15 mg |
4+4 |
| Mala
D |
Ethinyl estradiol |
0.03 mg |
Norgestrel |
0.30 mg |
4+4 |
| Mala
N |
Ethinyl estradiol |
0.03 mg |
Norgestrel |
0.30mg |
4+4 |
| Femilon |
Ethinyl estradiol |
0.02 mg |
Desogestrel |
0.15 mg |
5+5 |
| Pearl |
Ethinyl estradiol |
0.03 mg |
Norgestrel |
0.30 mg |
4+4 |
| Loette |
Ethinyl estradiol |
0.02 mg |
Levonorgestrel |
0.10 mg |
5+5 |
| Novelon |
Ethinyl estradiol |
0.03 mg |
Desogestrel |
0.15mg |
4+4 |
| Notes : |
*Triphasic pills should not
be used as EC to avoid miscalculation of dosage.
* Only white coloured tablets should be used while prescribing
Mala N, Mala D or Pearl as ECP (i.e. 28 pill packs where
red pills are non-hormonal iron tablets). |
|
Advantages :
universally available
women familiar with pills thus find
COC more acceptable
Disadvantages :
confusion about doses in different formulations
contraindications to estrogen use in
some women
higher probability of side-effects as
compared to LNG
2.5.2 Intrauterine device (IUD)
A trained healthcare provider can insert
a Copper T IUD within 5-7 days of unprotected sex.
This is the most effective EC method but
is not suitable for masses since infrastucture and training is required.
CuT use is undesirable in young nulliparous women or in women with
multiple sex partners. There is a risk of pelvic inflammatory disease
and subsequent infertility following CuT use especially in high-risk
women. Sometimes, irregular bleeding associated with IUD insertion
may mask diagnosis of early pregnancy.
Advantages :
- higher efficacy rates (over 99%)4
- very few compliance issues
- no systemic effects
- can be used as ongoing long-term contraception
- suitable for clients with history of
thrombo-embolic disease, stroke, heart attack and women who have
difficulty ingesting ECP due to vomiting
- may be suitable for women who present
later than 120 hours and before 7 days of unprotected intercourse
4 .
- can be used as a ‘third-chance’
when EC pill has been vomited or the woman is unable to take the
full dose due to intractable nausea or other side effects.
Disadvantages :
- unsuitable for women with multiple sex
partners and those with active reproductive tract infection
- relatively contraindicated in nulliparous
women
- not suitable for women with previous ectopic
pregnancy
- the infrastructure and trained personnel
may not be available everywhere
- irregular bleeding or spotting associated
with CuT insertion may be confused with bleeding due to abortion
or ectopic pregnancy and vice versa, delaying the diagnosis.
2.5.3 Mifepristone (RU-486)
These anti-progestins act as :
anti-implantation agents when given
post-coitally
menses-inducers when given in luteal
phase
abortifacients when given in early pregnancy
Mifepristone (RU486) has been found effective
in single dose of 600 mg, 50 mg and 10 mg when used as emergency
contraception7,12. Current accepted dose is 10 mg as
a single dose to be used within 120 hours of sexual exposure.
In comparative trial of RU 486 with Yuzpe
regimen, side-effects were less common with mifepristone but menstrual
disturbances were observed more often.
Advantages :
single dose
well tolerated with minimal side-effects
Disadvantages :
menstrual delay adds to anxiety in women
break-through ovulation may occur resulting
in failure if further sexual exposure occurs
higher risk of ectopic pregnancy
10 mg formulation is not available in
India
2.6
Special Consideration
2.6.1
Limitations
- the efficacy of emergency contraceptive
pills is influenced by the time elapsed since unprotected intercourse
and the time in a women’s cycle at which she had sex. The
earlier the ECP are taken after unprotected intercourse, the more
effective they are. The closer a woman is to ovulation at the
time of unprotected intercourse lower is the efficacy.
- the failure of ECP to prevent pregnancy
beyond the time-frame of efficacy window (120 hours) following
unprotected intercourse may limit it’s use in clients who
report later than this interval, as awareness is low.
- copper IUD (most effective method of
EC) is unsuitable for nullipara and clients at risk of STIs.
2.6.2 Safety of ECP
In more than 30 years of ECP use no deaths
or serious medical complications have been reported. The dose of
hormones is relatively small and the short exposure does not have
any metabolic effects.
The use is not associated with fetal malformations
or congenital defects.
ECP do not increase the risk of ectopic
pregnancy, but there may be a higher percentage of ectopic pregnancies
among failures, thus possibility of ectopic pregnancy is to be ruled
out in all cases of ECP failure.
2.6.3 Side-effects
There are no major side-effects reported.
A few temporary minor adverse events, which are not present usually
beyond 48 hours are listed in Table 5.
Some women also experience inter-menstrual
bleeding and altered menstrual cycles including heavier menstrual
bleeding (13.8%) or lighter bleeding (12.5%). Majority of women
(58%) will have their next menstrual period at the expected time
or within a few days of the expected date6.
Table
5 Incidence of common side effects
| |
(%
with symptoms) |
| Yuzpe |
LNG |
| Nausea |
50.5 |
23.1 |
| Vomiting |
18.8 |
5.6 |
| Dizziness |
16.7 |
11.2 |
| Fatigue |
28.5 |
16.9 |
| Headache |
20.2 |
16.8 |
| Breast tenderness |
12.1 |
10.8 |
| Low abdominal pain
|
20.9 |
17.6 |
| Other adverse events
(Diarrhoea, irregular bleeding & spotting) |
16.7 |
13.9 |
|
|